“For the first time ever the Danish mental health system has been found guilty of causing the death of one of its patients,’ writes Dorrit Cato Christensen, author of Dear Luise. “This is important news. One hopes that far more psychiatric healthcare providers will be found guilty of causing death with their dangerous treatment. The psychiatric ward where this patient was treated I know very well. My daughter Luise died there from overmedication.
“After the verdict the Clinic Manager claimed that they have learned from the sad story so treatment will be safer, with less medication. I don’t believe them at all,” says Dorrit. “They said exactly the same eight years ago when my beloved Luise died in their care. In our organization Death in Psychiatric Care we see how bad psychiatric treatment really is. People contact us constantly to tell us how a beloved relative who sought psychiatric help suddenly ends up as a dangerously ill zombie. Many report that a relative has died from overmedication.”
Translation of a January 9, 2014 article in Politiken, a leading Copenhagen-based daily newspaper, covering the ruling on Adel’s suicide:
Gross medical negligence led to suicide
Psychiatric Hospital in Amager harshly criticized for overmedicating 26-year-old man. Clinical Manager claims that incidents involving medicine in large doses have led to ‘cultural change’ in psychiatric treatment.
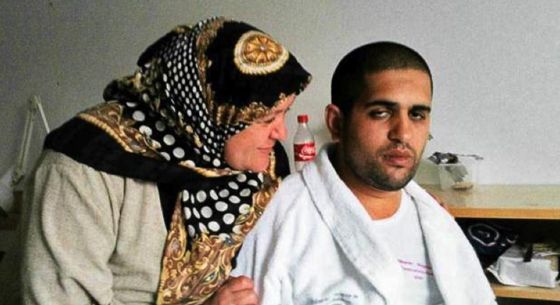
MANIC DEPRESSIVE. His brother says psychotropic drugs changed Adel from a vigorous 26-year-old to looking like “a 90-year-old patient in a hospice.” – Photo: PRIVATE PHOTO
By HANS DRACHMANN
A 26 -year-old psychiatric patient who committed suicide by throwing himself in front of a subway train in June 2011 had been so heavily medicated at the Psychiatric Center in Amager that the side effects were ‘unbearable.’
After two years of deliberations, the Patient Safety Commission has severely criticized the psychiatric hospital for providing treatment to the patient, Adel Saidane, which ‘did not meet generally accepted professional standards.’
Upheld all complaints
‘My older brother suffered so many side effects that were so unbearable that any human being might commit suicide in that situation.’ said the patient’s brother, Hafed Amin Saidane , who brought the case before the Patient Safety Commission.
The report criticized the Psychiatric Center on five specific points. The 26-year-old was overdosed with medication. The doctors did not given any reason for the high doses, as they should have. They failed to take proper care of the patient and were not sufficiently focused on side effects. The hospital ward should have provided Adel Saidane with an individual caretaker so he could not leave the center unaccompanied.
‘All our complaints have been upheld. We were in no doubt that he committed suicide because of the medication’s side effects,’ says Hafed Saidane.
His brother was bipolar but had not been hospitalized for two and a half years. Then in May 2011 he felt distressed and checked himself into the hospital. Over the next four weeks he was treated with several antipsychotics combined with sedatives in amounts that, in his brother’s words, changed him from a vigorous 26-year-old to looking like ‘a 90-year-old patient in a hospice.’
The case has consequences
At Copenhagen Metro Mental Health Services they’re deeply apologetic over the incident. ‘I take this very personally. We are so sorry and my heart goes out to the relatives. It’s a terrible thing and I feel awful about it,’ says Inger Merete Terp, Clinical Manager at Amager Psychiatric Center.
The case is an example of the wide-ranging practice of overmedicating psychiatric patients, which was prevalent in the Copenhagen area until mid-2012, when Politiken began covering the situation.
Overmedication, among other things, led to the dismissal of a Clinical Manager in Glostrup and a reprimand to a deputy director of Copenhagen Metro Mental Health, prompting the adoption of an action plan mandating close monitoring of medication to prevent overdoses.
Subsequently the proportion of patients treated with heavy doses of the antipsychotic Zyprexa was reduced from almost 25 percent to about 5 percent.
‘I think we’ve got a good grip on it and we’ve now ensured that action can be taken on the same day if any mental health center starts prescribing excessive doses,’ says Svend Hartling , vice president of Metro Mental Health.
He describes the Amager incident as ‘highly irregular’ and will now ask the executive board of Metro Mental Health whether enough has been done to prevent this from happening again.
Paradigm shift
The Patient Safety Commission’s report is also being sent to the National Board of Health and to chief medical officers in Copenhagen, who will address the issues at a meeting next week.
‘We are discussing whether there should be consequences, so other patients are not put at risk,’ said National Health Board oversight manager Anne Mette Dons. She is generally satisfied that the Metro region has taken effective action against overmedication. ‘There really a has been a paradigm shift.’
Clinic Manager Inger Merete Terp says that the overmedication case has resulted in a ‘culture change.’
‘We need to focus not only on medication but also on patients’ daily lives. We must look at patients’ daily life, see that they can wash dishes or take a walk and do things that contribute to quality of life,’ she says.
The Commission’s ruling will now be taken up with doctors at Amager Psychiatric Center and with other mental health center managers in the Metro Area.

